IVF is one of the most recognised assisted reproductive technologies, but many people still ask about the full meaning of IVF, how the treatment works, and what to expect at each stage. This guide explains the definition, the medical context, and the complete IVF procedure—from preparation and medication to egg retrieval, fertilisation, embryo transfer, and pregnancy testing. You will also find a practical day-by-day outline, plus an overview of advanced options that build on core methods.
What Does IVF Mean?
Full meaning of IVF in medical terms
The full meaning of IVF is in-vitro fertilisation. In medical terms, IVF describes a clinical process where eggs are collected from the ovaries and fertilised with sperm outside the human body in a controlled laboratory environment. The resulting embryos are then placed into the uterus with the intention of achieving pregnancy. Because fertilisation occurs in a lab dish or chamber, IVF is classified as an assisted reproductive technology (ART). In short, the meaning of IVF in medicine is a laboratory-assisted pathway to conception that bypasses the need for fertilisation within the fallopian tube.
Patients sometimes ask for the full meaning of IVF in medical terms or the full meaning of IVF in a medical term context; both point to the same definition—fertilisation in a laboratory setting, followed by embryo transfer into the uterus. If you are comparing definitions across sources, remember that “in-vitro” literally means “in glass,” a historical reference to lab glassware.
IVF meaning in pregnancy and fertility treatment
When people ask about IVF meaning in pregnancy, they want to know how the lab step translates into a typical pregnancy. Once an embryo created through IVF implants into the uterine lining, the pregnancy proceeds like any naturally conceived pregnancy. That is why many patient guides use phrases such as “procedure for IVF pregnancy” or “IVF process for pregnancy” to emphasise that the aim is a healthy implantation and ongoing gestation. For a broader overview of indications, protocols, and outcomes, see our summary of IVF Treatment.
IVF abbreviation explained
Patients also search for the IVF meaning of abbreviation or IVF meaning abbreviation: IVF stands for In-Vitro Fertilisation. In day-to-day language, questions such as “what IVF stands for,” “what is the meaning of IVF,” “what is the full meaning of IVF,” or even “what is the meaning of IVF in pregnancy” all point back to this same abbreviation and definition. Although you might encounter colloquial queries like “what do you mean by IVF” or “what is IVF mean medical term,” the precise phrasing is: IVF means in-vitro fertilisation, a medical procedure to assist conception.
The IVF Process Step by Step
Understanding the process helps transform anxiety into a plan. Below is the complete IVF procedure explained step by step—the process of in-vitro fertilisation from start to finish.
Preparation before IVF treatment
Before any medication begins, the clinic confirms the clinical picture and prepares a safe plan. Typical steps include:
- Medical history, pelvic ultrasound, and hormone tests.
- Semen analysis to assess count, motility, and morphology.
- Infectious disease screening where indicated.
- Lifestyle guidance (healthy weight, nutrition, sleep, cessation of smoking).
- Review of consent forms and timetable.
This stage ensures the in-vitro fertilization treatment process is tailored to you. It is the foundation for the IVF process from start to finish and sets timing for scans, injections, and lab work.
Ovarian stimulation and medication for IVF procedure
The first active phase is ovarian stimulation. Medication for IVF procedure—usually gonadotropins such as FSH with or without LH—encourages multiple follicles to develop at once. A clinic-specific IVF med schedule sets exact doses and times. You will attend monitoring every 1–3 days for ultrasound and blood tests; the team adjusts medication according to follicle growth and hormone levels. This part of the day by day IVF process typically lasts 8–12 days.
While most people continue normal life, expect mild bloating, breast tenderness, or mood changes. Hydration and gentle movement can help.

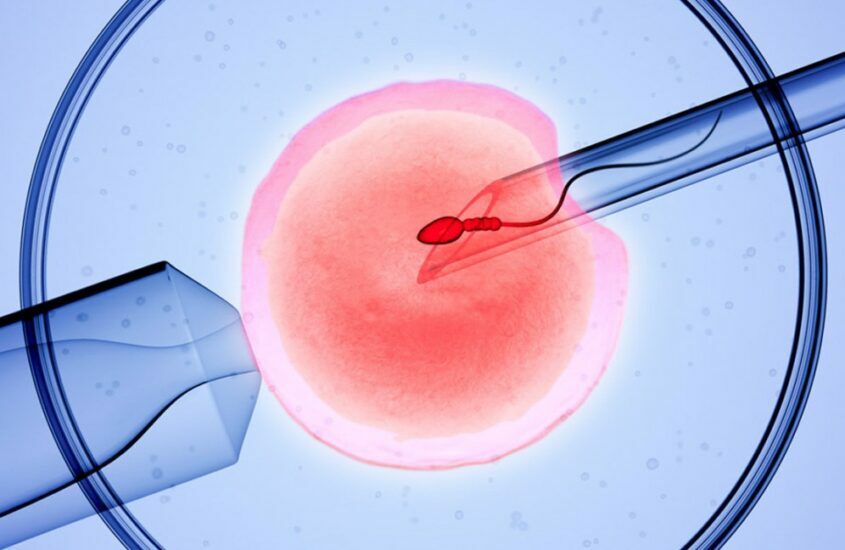
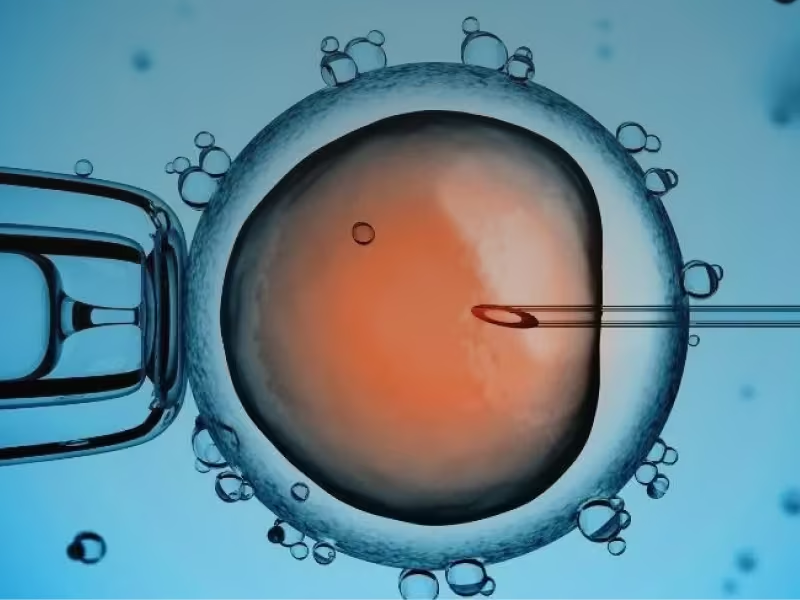
Egg retrieval and fertilisation in the lab
When several follicles reach the target size, a trigger injection matures the eggs. About 36 hours later, egg retrieval takes place—usually a 15–30 minute outpatient procedure under light sedation. Immediately afterward, the IVF lab process begins. Fertilisation can be:
- Conventional IVF: eggs and processed sperm are co-incubated.
- ICSI: a single sperm is injected directly into each mature egg.
The laboratory confirms fertilisation the next day and continues the in-vitro fertilisation IVF process of culture and quality assessment.
Embryo development and transfer
Embryos are cultured for three to five days. On day 3, many embryos are at the cleavage stage (6–8 cells). By day 5, the strongest may reach the blastocyst stage, which often offers clearer selection for transfer. Depending on your plan, one or two embryos are transferred into the uterus using a thin catheter. The transfer is quick and usually painless. Remaining good-quality embryos can be frozen for future use.
The two-week wait and pregnancy testing
After transfer, you enter the two-week wait while the embryo attempts implantation. During this period, clinics often perform blood tests to monitor hormone levels (such as progesterone and oestrogen, and in some cases early hCG) to optimise support for implantation. The official pregnancy test (β-hCG) is usually scheduled 9–12 days after a day-5 transfer or 12–14 days after a day-3 transfer. This phase represents the handover from laboratory work to the body’s natural implantation and early development.
IVF Procedure Day by Day – What to Expect
Patients often want an IVF procedure day-wise view—the outline of the process of IVF from start to finish on a calendar. Here is a representative example (timing varies):
DayStageWhat happensTips1–3Stimulation beginsStart injections per IVF med scheduleSet phone reminders4–7MonitoringUltrasound and bloods; dose adjustmentsHydrate; light activity8–12Late stimulationFollicles approach target sizeAvoid vigorous workouts13–14TriggerPrecisely timed injectionPlan transport for retrieval15Egg retrievalShort procedure under sedationArrange a companion home15–19Lab cultureFertilisation confirmed; embryo growthAsk when lab updates arrive18–20Embryo transferDay 3 or day 5, fresh or frozenResume gentle routine20–34Two-week waitImplantation window; test scheduled, hormone monitoringAttend scheduled blood tests and follow clinic advice
IVF process for females
The IVF process for females focuses on stimulation, retrieval, and transfer. The team closely observes your response to reduce risks such as ovarian hyperstimulation. Clear instructions, an accurate IVF calendar, and timely communication with nurses are your best tools.
IVF process for pregnancy outcomes
The IVF process for pregnancy aims to create and place a viable embryo in a receptive uterus. Success depends on egg and sperm quality, embryo development, and endometrial readiness. Modern lab techniques—careful culture conditions, blastocyst transfer, and vitrification—help optimise the odds.
IVF process from start to finish
From first consultation to confirmed test, the process of IVF in humans typically spans one menstrual cycle once stimulation begins. Including preparation and recovery, many people find that the full journey takes 4–8 weeks. If you are deciding between paths, our overview of IVF Treatment explains timelines and choices.
Advanced IVF Methods and Technologies
The field evolves quickly, so you will also see questions such as “IVF technology meaning,” “IVF lab process innovations,” or “future of IVF technology.” Several options sit on top of the core process:
Egg freezing and fertility preservation
Egg freezing (oocyte cryopreservation) lets you preserve eggs for later use. It is especially helpful for medical reasons (e.g., before chemotherapy) or for personal timing. You may complete stimulation and retrieval now, then fertilise and transfer embryos in the future. For details about indications and steps, visit our page on Egg Freezing.
Genetic testing and advanced IVF treatments
Some patients choose embryo testing to screen for chromosomal abnormalities or specific conditions. Preimplantation genetic testing (PGT) can be used with blastocyst biopsy; embryos are then frozen while results are analysed. This belongs to the family of advanced options described in Advanced Treatments IVF. The goal is to improve selection and reduce the chance of transferring aneuploid embryos.
Future of IVF technology
Emerging areas include AI-assisted embryo selection, non-invasive genetic assessment via spent media, better time-lapse imaging, and refinements to freezing and thawing protocols. These innovations don’t change the definition of IVF, but they can influence success rates and how clinics explain the process in vitro fertilisation to patients.
Final Thoughts: Understanding IVF Meaning and Process
Breaking down IVF—its meaning and process—helps you move from uncertainty to action. The full meaning of IVF is in-vitro fertilisation, but behind the abbreviation stands a carefully managed series of steps designed to maximise the chance of a healthy pregnancy: stimulation, monitoring, egg retrieval, fertilisation, embryo culture, transfer, and testing. If you prefer a concise outline, think of it as the IVF process from start to finish on a calendar—an organised path rather than an unknown.
If you are weighing options, start with our overview of IVF Treatment. If you are planning ahead, consider whether fertility preservation via Egg Freezing or other Advanced Treatments IVF fits your goals. With a clear process, precise schedules, and an informed team, your path through IVF becomes easier to navigate.


.webp)

%201.png)






.webp)
.webp)
.webp)
.webp)
.webp)



